Ovaries usually produce hormones and eggs until the early fifties, but in some cases, women can enter early menopause because of Ovarian Insufficiency or Failure (POF) and they enter menopause.

Stem Cells Treatment for Premature Ovarian Failure (POF)
Symptoms
- Irregular or skipped periods, which might be present for years or develop after a pregnancy or after stopping birth control pills
- Difficulty getting pregnant
- Hot flashes
- Night sweats
- Vaginal dryness
- Dry eyes
- Irritability or difficulty concentrating
- Decreased sexual desire
Causes
- Genetic disorders are associated with primary ovarian insufficiency.
- Chemotherapy and radiation therapy.
- Cigarette smoke, chemicals, pesticides and viruses.
- immune system response to ovarian tissue
Risk factors
- Age. The risk goes up between ages 35 and 40.
- Family history. of Primary Ovarian Insufficiency increases the risk.
- Surgeries involving the ovaries increase the risk of POI.
Complications
- Infertility Inability to get pregnant.
- Osteoporosis Low levels of estrogen increase the risk .
- Depression or anxiety related to risk of infertility and complications from estrogen level.
- Heart disease Early loss of estrogen might increase the risk.
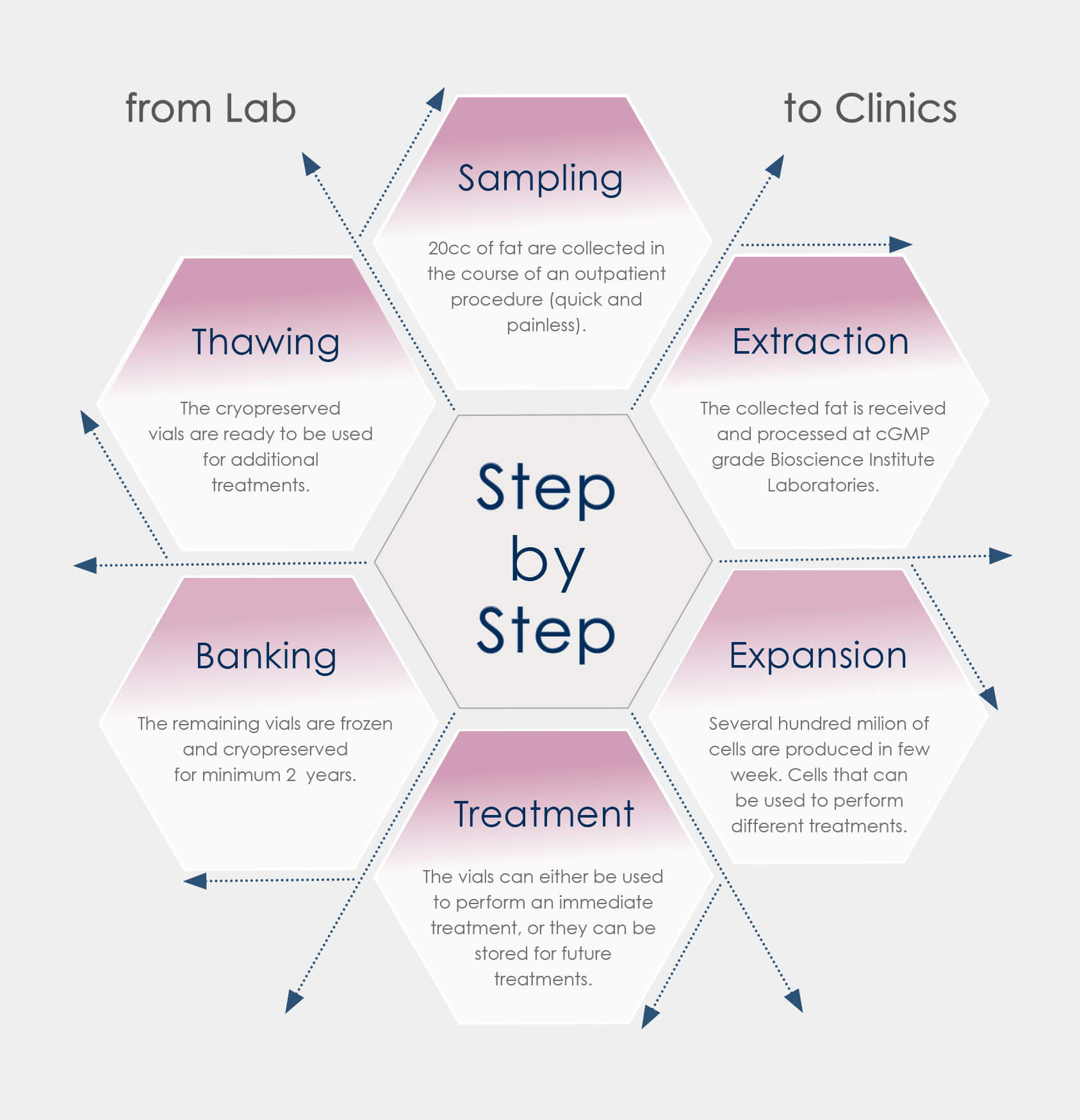
Stem Cell Therapy the Procedure
- collection of only 20 cc of fat biopsy
- isolation and expansion of the stem cells (in two weeks)
- treatment: intra-ovarian injection of Stem cells
- the cells not utilized are cryopreserved and can be used for other treatments
Results & References
- “After MSC therapy, the sizes of the ovaries returned to normal and the endometrial thickness was increased, along with rich endometrial blood flow, suggesting that stem cell therapy may be an effective therapeutic strategy for the treatment of POF”
- “stem cell transplantation not only resulted in improvement of the hormonal profile of a POF patient but also in the resuming of menstruation and the occurrence of pregnancy, resulting in the delivery of a full-term healthy infant”
EXPERIMENTAL AND THERAPEUTIC MEDICINE 15: 4105-4118, 2018
- It is evident that stem cell therapies have potential in treating POI. Stem cells and their exosomes, including content such as miRNAs, show positive effects in enhancing and restoring various aspects of ovarian function, such as folliculogenesis, the GC apoptosis rate, vascular formation, and genetic stability.
J Ovarian Res. 2020; 13: 74.
Scientific evidence
ADSC transplantation in women with premature ovarian failure following chemotherapy was shown to induce ovarian function recovery, improving both hormones production and ovarian structure. It improves endometrial thickness too, and was associated with a richer blood signal in the endometrium. In a study on idiopathic premature ovarian failure, autologous stem cell transplantation allowed ovulation in 60% of treated women. In another study, menstruation restarted 3 months after stem cell therapy in 20% of treated women, which regained ovarian reserve and the secretory function of a previously atrophic endometrium. The treatment allowed a woman to get pregnant and to give birth to a full-term healthy baby. Finally, preliminary results of the ROSE (Rejuvenation of Premature Ovarian Failure With Stem Cells) clinical trial demonstrated that in women who completed autologous stem cell therapy serum estrogen levels increased 3 months after stem cells injection. The effect lasted for at least 1 year, menopausal symptoms were alleviated, and menstruations resumed 6 months after the injection.

Bibliography
Haahr MK et al. EBioMedicine. 2016 Jan 19;5:204-10. doi: 10.1016/j.ebiom.2016.01.024
Haahr MK et al. Urology. 2018 Nov;121:203.e6-203.e13. doi: 10.1016/j.urology.2018.06.018

